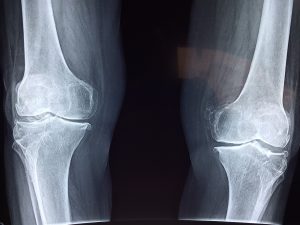
In this study showing evidence of knee cartilage growth after autologous adipose tissue injection, Dr. Jaewoo Pak and colleagues enrolled three patients: an 87-year-old female with stage 3 OA, a 68-year-old male with stage 3 OA, and a 60-year-old female with stage 3 OA, were included. All had significant findings of advanced osteoarthritis on MRI, all had a significant disability with range of motion and walking, and all had been told their only option was total knee replacement. All three patients were treated with autologous adipose and autologous PRP and HA at day 0. Subsequently, the patients returned to the clinic every week × 3 for HA and autologous PRP activated with calcium chloride. The patients were assessed at the weeks of 2, 4, and 16 (18 or 22) for pain improvement in terms of VAS and function improvement in terms of physical therapy parameters. In addition, these patients were followed by post-treatment MRI 3 months after the treatment. All patients demonstrated improvement in cartilage on MRI, and all patients reported greater than 75% improvement in pain and range of motion by 22 weeks.
More evidence of knee cartilage growth after Adipose Biocellular tissue injection.
Regeneration of Cartilage in Human Knee Osteoarthritis with Autologous Adipose Tissue-Derived Stem Cells and Autologous Extracellular Matrix
Jaewoo Pak, Jung Hun Lee, […], and Sang Hee Lee
Abstract
This clinical case series demonstrates that percutaneous injections of autologous adipose tissue-derived stem cells (ADSCs) and homogenized extracellular matrix (ECM) in the form of adipose stromal vascular fraction (SVF), along with hyaluronic acid (HA) and platelet-rich plasma (PRP) activated by calcium chloride, could regenerate cartilage-like tissue in human knee osteoarthritis (OA) patients. Autologous lipoaspirates were obtained from adipose tissue of the abdominal origin. Afterward, the lipoaspirates were minced to homogenize the ECM. These homogenized lipoaspirates were then mixed with collagenase and incubated. The resulting mixture of ADSCs and ECM in the form of SVF was injected, along with HA and PRP activated by calcium chloride, into knees of three Korean patients with OA. The same affected knees were reinjected weekly with additional PRP activated by calcium chloride for 3 weeks. Pretreatment and post-treatment magnetic resonance imaging (MRI) data, functional rating index, range of motion (ROM), and pain score data were then analyzed. All patients’ MRI data showed cartilage-like tissue regeneration. Along with MRI evidence, the measured physical therapy outcomes in terms of ROM, subjective pain, and functional status were all improved. This study demonstrates that percutaneous injection of ADSCs with ECM contained in autologous adipose SVF, in conjunction with HA and PRP activated by calcium chloride, is a safe and potentially effective minimally invasive therapy for OA of human knees.
Thinning hair? PRP to the rescue!
The Science of How Your Stem Cells Can Restore Damaged Joints
Avoiding Knee Surgery: 2-year PRP Study Confirms Cartilage Repair in Osteoarthritis of the Knee
Osteoarthritis Treatment: The ultimate game plan
Regenerative Injection Recovery: Exercise guidelines to help you get the most from your treatments
Chondroitin sulfate plus glucosamine as effective as Celebrex